About Pancreatic Cancer
What Is Pancreatic Cancer?
 Pancreatic cancer begins when abnormal cells in the pancreas grow and divide out of control and form a tumor.
Pancreatic cancer begins when abnormal cells in the pancreas grow and divide out of control and form a tumor.
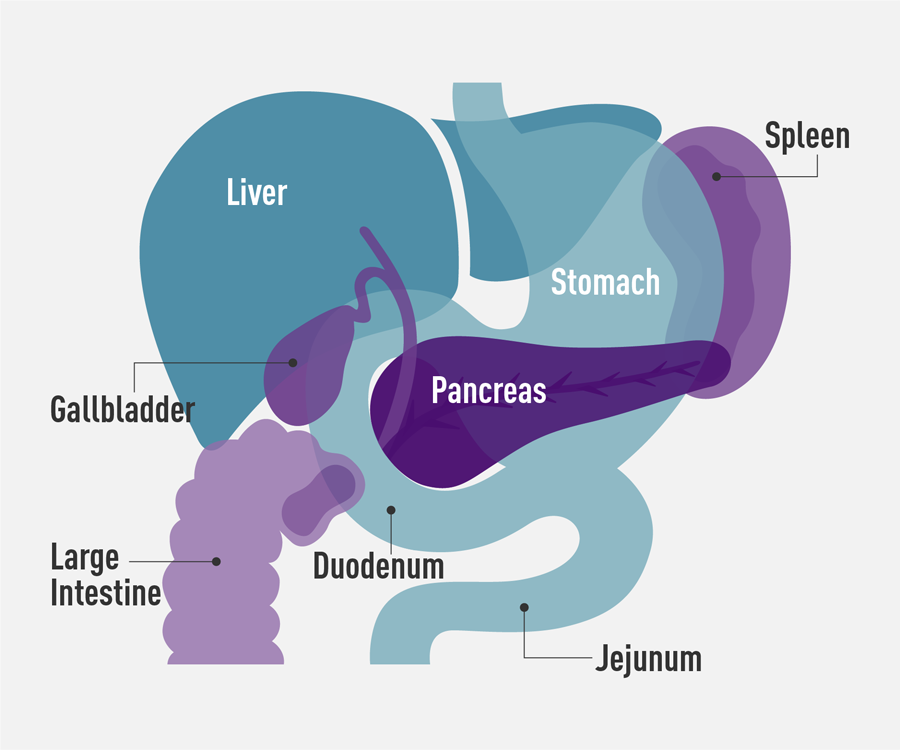
The pancreas is a gland located deep in the abdomen, between the stomach and the spine. It makes enzymes that help digestion and hormones that control blood-sugar levels.
Organs, like the pancreas, are made up of cells. Normally, cells divide to form new cells as the body needs them. When cells get old, they die, and new cells take their place.
Sometimes this process breaks. New cells form when the body does not need them, or old cells do not die. The extra cells may form a mass of tissue called a tumor.
Some tumors are benign. This means they are abnormal but cannot invade other parts of the body.
A malignant tumor is called cancer. The cells grow out of control and can spread to other tissues and organs.
Even when the cancer spreads to other areas of the body, it is still called pancreatic cancer if that is where it started. Pancreatic cancer often spreads to the liver, abdominal wall, lungs, bones and/or lymph nodes.
Order our free educational packet for more information about pancreatic cancer and its treatment.
How Many People Will Get Pancreatic Cancer?
More than 64,440 Americans are expected to be diagnosed with pancreatic cancer in 2024. That is 182 people diagnosed every day.
Pancreatic cancer is the 10th most commonly diagnosed cancer in the U.S.
Types of Pancreatic Cancer
Pancreatic tumors are either exocrine or neuroendocrine (endocrine) tumors. This is based on the type of cell they start in. Knowing the type of tumor is important because each type acts differently and responds to different treatments.
More than 90% of pancreatic cancers are exocrine tumors. The most common type of pancreatic cancer is adenocarcinoma.
Less than 10% of pancreatic tumors are neuroendocrine tumors (pancreatic NETs or PNETs), also called islet cell tumors. They often grow slower than exocrine tumors.
Learn about the types of pancreatic cancer.
What Causes Pancreatic Cancer?
Changes in your DNA cause cancer. These can be inherited from your parents or can arise over time. The changes that arise over time can happen because you were exposed to something harmful. They can also happen randomly.
Pancreatic cancer's exact causes are not well understood. About 10% of pancreatic cancers are considered familial or hereditary. Most pancreatic cancer happens randomly or is caused by things such as smoking, obesity and age.
If you are a first-degree relative of someone diagnosed with pancreatic cancer, you may have an increased risk of developing pancreatic cancer. Your family member with pancreatic cancer is strongly recommended to undergo genetic testing for inherited mutations.
- Negative results often mean you do not need to get genetic testing.
- If the results are positive, unknown or if you have several close family members with cancer, the Pancreatic Cancer Action Network recommends you consult with a genetic counselor to determine if you should get genetic testing for inherited cancer risk and if you should discuss options for monitoring.
A person may also be more likely to get pancreatic cancer because of:
- Long-standing diabetes
- Chronic and hereditary pancreatitis
- Smoking
- Race (ethnicity): African-American or Ashkenazi Jew
- Age: over the age of 60
- Gender: males slightly more likely
- Diets high in red and processed meats
- Obesity
This does not mean that everyone who has these risk factors will get pancreatic cancer or that everyone who gets pancreatic cancer has one or more of these.
Learn more about pancreatic cancer risk factors.
Signs and Symptoms of Pancreatic Cancer
Pancreatic cancer may cause only vague, unexplained symptoms, such as:
- Pain, usually in the abdomen or back
- Weight loss
- Jaundice (yellowing of the skin, eyes or both) with or without itching
- Loss of appetite
- Nausea
- Changes in stool
- Pancreatitis (swelling of the pancreas)
- Recent-onset diabetes
If you are experiencing one or more of these symptoms, we urge you to speak to your doctor immediately and reference pancreatic cancer.
Fatigue, weakness and depression are also symptoms. A person with advanced pancreatic cancer may also have fluid in the abdomen and blood clots.
Learn more about pancreatic cancer signs and symptoms.
How Is Pancreatic Cancer Diagnosed?
A pancreatic tumor can only be seen on an imaging study such as a computed tomography (CT) scan, magnetic resonance imaging (MRI) or endoscopic ultrasound (EUS). Then, the doctor gets a sample of the tumor tissue to figure out the exact diagnosis.
Why Is Pancreatic Cancer Hard to Find?
The pancreas is located deep in the abdomen, so doctors usually cannot see or feel the tumor during a physical exam. Also, pancreatic cancer symptoms are not always obvious and usually develop over time.
Doctors may use several tests to make a diagnosis. But, there is no standard test to diagnose pancreatic cancer. This makes diagnosis even more complicated.
What Treatments Exist for Pancreatic Cancer?
Pancreatic cancer treatment depends on the stage of the disease and the patient's general health. Patients may get standard (approved) treatments or take part in clinical trials.
Standard treatments are surgery, chemotherapy and radiation. Clinical trials study new treatments. The Pancreatic Cancer Action Network strongly recommends clinical trials at diagnosis and during every treatment decision.
Why Is Pancreatic Cancer Hard to Treat?
Surgery offers the best chance of controlling pancreatic cancer for a long time. But, most patients are diagnosed at later stages and are not eligible for surgery. Tests to find pancreatic cancer in the earliest stages are urgently needed.
As early detection study continues and as technology gets better, researchers predict that we will make progress toward finding the disease earlier.
Another challenge is that pancreatic tumors are surrounded by a dense tissue layer, called the stroma. This makes it difficult for treatment to reach the tumor. Researchers are studying ways to get treatment through the stroma to make it more effective.
Also, some cancers have been successfully treated with targeted therapies which block specific mutations. But, these drugs have not been developed specifically for pancreatic cancer yet.
Biomarker testing of tumor tissue and genetic testing for inherited mutations tell you about your unique biology. Results may align with targeted treatments that work well in other cancer types. As more studies are done, more targeted treatments will be developed and approved for pancreatic cancer patients who have specific genetic changes.
PanCAN Is Here to Help
For free, in-depth and personalized resources and information on pancreatic cancer, contact PanCAN Patient Services.
Information reviewed by PanCAN's Scientific and Medical Advisory Board, who are experts in the field from such institutions as University of Pennsylvania, Memorial Sloan-Kettering Cancer Center, Virginia Mason Medical Center and more.
Information provided by the Pancreatic Cancer Action Network, Inc. (“PanCAN”) is not a substitute for medical advice, diagnosis, treatment or other health care services. PanCAN may provide information to you about physicians, products, services, clinical trials or treatments related to pancreatic cancer, but PanCAN does not recommend nor endorse any particular health care resource. In addition, please note any personal information you provide to PanCAN’s staff during telephone and/or email communications may be stored and used to help PanCAN achieve its mission of assisting patients with, and finding cures and treatments for, pancreatic cancer. Stored constituent information may be used to inform PanCAN programs and activities. Information also may be provided in aggregate or limited formats to third parties to guide future pancreatic cancer research and education efforts. PanCAN will not provide personal directly identifying information (such as your name or contact information) to such third parties without your prior written consent unless required or permitted by law to do so. For more information on how we may use your information, you can find our privacy policy on our website at pancan.org/privacy.




